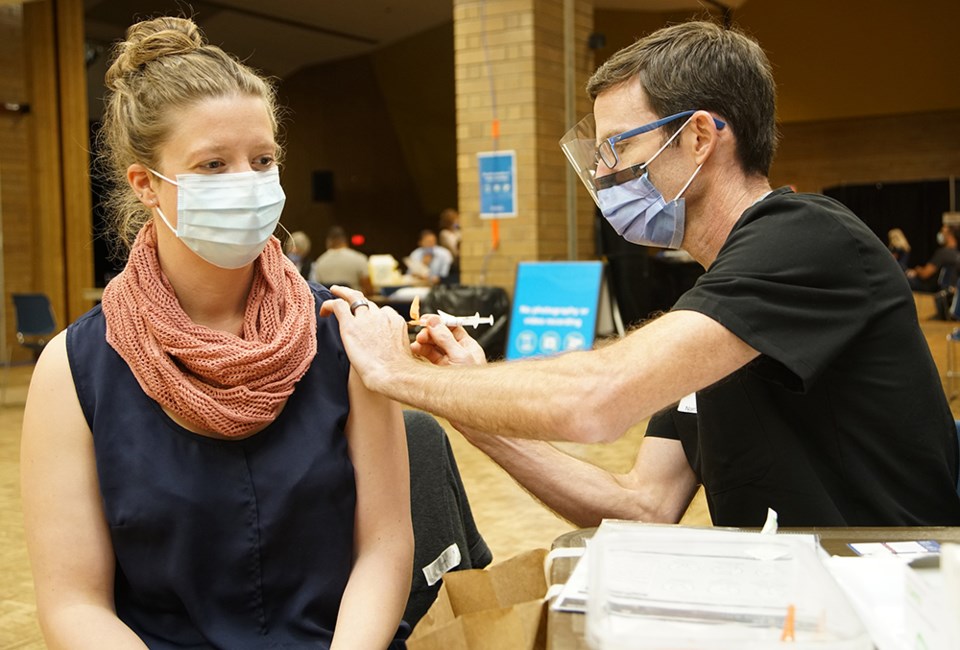
The pandemic has turned our world upside down. The past year has been filled with uncertainty, loss and worry. But it has also been a year of innovation, global cooperation and courage.
It hasn’t been perfect, and it’s not over yet, but much has been accomplished. More than 50 per cent of people in our area have now had their first COVID-19 vaccine. However, there are still people who are unsure about getting vaccinated.
They may wonder if it’s really necessary, particularly if they feel they are at low risk personally. There is so much information and misinformation online, it can be difficult to make an informed decision.
An important factor in the decision-making process is risk assessment. What is the risk of remaining susceptible to COVID-19 when compared with the risk of vaccination? And are there any additional benefits to vaccination?
What are the risks of COVID-19?
About 1.3 million Canadians (roughly one in 30) have been diagnosed with COVID-19 since the start of the pandemic, and more than 25,000 have died (about one in 50 confirmed cases).
Contrary to what many believe, it’s not only those over 65 who are at risk. According to Health Canada, as of May 14, 2021, more than 20,000 people under 60 had been hospitalized in Canada due to COVID-19 (accounting for more than one third of all COVID hospitalizations). Risk of death increases with every decade of life, from rare in children under 10, to about one in five for people over 80.
Independent of age, many common conditions such as high blood pressure, asthma, diabetes and obesity make people more likely to get seriously ill or die from COVID-19. Those who do become critically ill are more likely to have long-term organ injury (heart and lung damage) than those with milder illness.
COVID-19 is about 10 times more deadly than most typical influenza strains and much more infectious. Variants of concern - those strains considered more infectious - now make up about 80 per cent of cases in BC.
We are still learning about the long-term effects of COVID-19, but symptoms may last weeks or months, even in those who are younger, had no preexisting conditions and had relatively mild infections. Persistent symptoms of “long haulers” may include shortness of breath, cough, fatigue, joint pain and cognitive problems (brain fog) that can significantly affect quality of life.
Protection from serious or lasting illness
According to the BCCDC, a small percentage of people may still get COVID-19 after vaccination. This is most common within two to three weeks after vaccination, and much less likely after the second dose.
All vaccines used in Canada are known to provide a high level of protection against serious illness and death from COVID, even after one dose. So far, the vaccines are showing excellent effectiveness against current circulating strains of COVID-19 in BC, variants included.
Reducing the spread
Vaccinations may not completely eliminate COVID-19, but we have seen that as more people get vaccinated, the spread of the disease has slowed dramatically. Because vaccines help to stop the spread of the virus the risk of new variants emerging is also reduced. Everyone who gets vaccinated plays a part in ending the pandemic. If we can limit the serious impacts of COVID, then restrictions can be relaxed, too.
Health Canada estimates it will be safe to significantly lift restrictions once 75 per cent of eligible people in any given area have received their first dose, and at least 20 per cent have received their second dose.
What about vaccine safety?
All vaccines, past and present, can cause side effects because they stimulate our immune systems. Decades of experience with vaccines have shown that when side effects do occur, they typically arise in the first few weeks.
Most side effects people experience are minor, normal immune reactions, lasting one or two days (sore arm, low-grade temperature, headache or fatigue).
Rarely more serious symptoms, such as allergic reactions, may occur. According to the Public Health Agency of Canada, as of May 7 more than 15 million doses of vaccine had been administered in Canada. Of those, there were 872 reports of serious adverse effects (about one in 17,000 vaccinated), and most of these were not life-threatening. Generally the risks from vaccination are much lower than the risks posed by COVID-19.
Both the Johnson & Johnson and AstraZeneca vaccines have been associated with a rare but serious immune reaction causing blood clots (currently estimated at one per 50,000 to 100,000 doses). In BC, supply of these vaccines has diminished and they are no longer being offered for first doses. We now have much larger supplies of mRNA vaccines (Pfizer, Moderna) and everyone 18 years and older is now able to register and book an appointment for one of these. See prcomplexclinic.com for more info on second doses.
Risk in the Powell River area
Our relative isolation may have provided us with some protection over the past year. However, when we look at the reality of the pandemic in other isolated communities in Canada and around the world we know we are not immune to the effects of COVID-19. As travel restrictions are lifted we will become more susceptible and exposed, whether or not we are travelling outside the community.
Ultimately it is a personal decision whether or not to get vaccinated. It is up to each of us to do our research and assess our own risk. That is why it’s so important to have access to the most current, accurate information available. Recommended sources of reliable, accurate information include Canada.ca, vch.ca, bccdc.ca and immunizebc.ca. For local information visit prcomplexclinic.com/vaccines, or talk to your doctor or nurse practitioner.